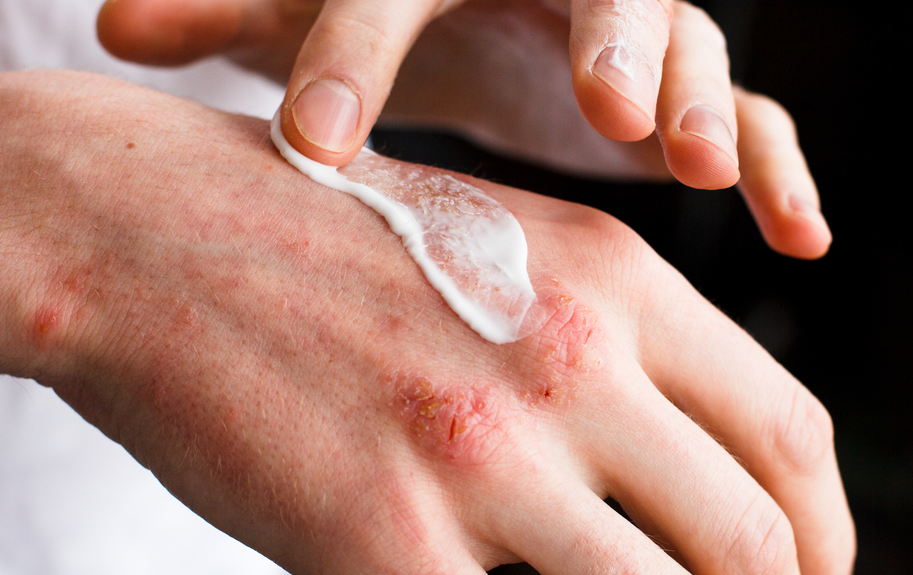
Introduction:
Atopic dermatitis (AD) refers to the development of spontaneous rash, scratching, and itching of the skin. The condition is also popular as Eczema. It is a prevalent skin condition in childhood which is believed to continue into adulthood in some cases. The symptoms of atopic dermatitis (AD) are at times so severe that some people might be vulnerable to the adverse impact of itching and scratching associated with it. Therefore, in such circumstances seeking help is the best thing one can do for themselves. Various Clinical Research Organizations are dedicated to conducting clinical trials for skin conditions that may help in finding potential treatment options.
Symptomatic Manifestation of Atopic Dermatitis:
Atopic dermatitis (AD) is chronic in origin, with the persistence of symptoms such as; inflammation, redness, and itching. Fortunately, a variety of viable treatment options are available to subside the discomfort associated with AD.
Coping with the consequences of Atopic Dermatitis is a tough task. Moreover, another complexity associated with the disease is finding the root cause of the disease. Little do most people know of the several factors such as environmental influence, genes, and immune system to be the culprit?
Put simply, Atopic Dermatitis is a noncontagious type of disease, expected to appear mostly during childhood. This doesn’t define atopic dermatitis (AD) as a disease of childhood, instead, it may be elicited irrespective of age.
The commonly reported manifestations of atopic dermatitis (AD) consonant with itching, scratching, and inflammation are:
- Swelling
- Cracking
- Weeping of clear fluid
- Crusting
- Scaling
Some other commonly reported clinical presentations of atopic dermatitis (AD) patients are:
- Red and dry patches of skin
- Rashes may ooze, and leak a clear fluid when scratched
- Thickening and hardening of the skin
- People with darker skin tones (increased melanin) often experience darkening or lightening of the skin in areas of skin inflammation
The characteristic distributive pattern of AD in terms of appearance and location varies with age. This doesn’t confine the rash to any particular site of the body with age. However, the symptoms can flare in multiple areas of the body at the same time and can appear in the same locations or new locations without warning.
Causes of Atopic Dermatitis (AD):
Atopic Dermatitis owns a substitute name (Atopic Eczema) for it. According to researchers, a combination of factors disrupting the moisture-controlling capacity of the skin leads to dry skin. The presence of dry skin is an explicit trademark of eczema or atopic dermatitis (AD).
A list of factors influencing dry skin are:
- The mutation changes in genes
- Problems with the immune system
- Exposure to certain things in the environment
Other potential causes are:
- Food allergies
- Soaps
- Compounds present in detergents, soaps, and some skin care products
- Stress
- Weather changes
- Hypersensitivity of the immune system to fight off bacteria, viruses, etc
- Exposure to tobacco smoke
- Air pollution
- Excessively dry skin
Diagnostic Criteria:
There are no standard criteria or checklists to identify symptoms persistent with AD. However; to rule out the disease you should seek medical advice from your practitioner at your earliest.
Some of the commonly enquired questions to determine the disease are:
- Does the rash itch? And where does it appear?
- The onset of symptoms first began?
- Do the flare-ups arise continuously or intermittently?
- Family history of atopic eczema
- Any other allergic conditions identified as of yet, such as allergies or asthma
- Do you believe your diet or lifestyle may be contributing to your symptoms?
Typically, to be diagnosed with atopic eczema you must have had a complaint of itchy, dry skin condition in the last 12 months.
Also read: Common cause of Breast Eczema
Correlation of Incidence with Ethnicity:
As stated previously, the occurrence of the disease is not determined by age. A certain link exists between the incidence of AD and the Non-Hispanic community. To begin with, research shows that the chance of developing AD is slightly higher in Non-Hispanic women, black children, and girls than in men and boys. In addition, another factor advocated for the incidence of AD is a family history of atopic dermatitis, hay fever, or asthma.
Commonly Affected Sites According to Age Group:
- From infancy up to 2 years of age a classic red rash with oozing and crusting is commonly expected to arise on the face, scalp, and skin traces surrounding the bending areas of the joint.
Diaper rash is often mistaken for AD by many parents. Therefore, for your understanding, the condition doesn’t prevail in such areas.
- In children aged 2 years up to puberty, the presence of a thickened red rash, which may ooze or bleed when scratched, is common in the folds of elbows and knees, neck, and ankles.
- During the teenage and adult years of life, a red to dark brown scaly rash, which may bleed and crust when scratched is expected to appear on the hands, neck, elbows, and knees, around the eyes, ankles, and feet.
Concomitant Occurrences of Other Diseases with Atopic Dermatitis are:
Understanding the potential triggers of atopic dermatitis (AD) is essential for the resolution of AD flares. But there is more to it. For instance, you may be someone dealing with undiagnosed concomitant diseases eliciting flares or mimicking AD symptoms:
- Allergies
- Hay fever
- Asthma
- Sleep disturbance
- Cardiovascular disease
- Ichthyosis
Treatment:
While the origin of AD is multifactorial there is no mainstay of treatment available to cure the disease. Thereafter, certain lifestyle modifications, and avoiding exposure to triggers are essential cornerstones of a comprehensive management regimen. Here are some commonly used treatment options for atopic dermatitis:
- Moisturizers: Using a moisturizer regularly can help keep the skin hydrated and prevent dryness and itching.
- Topical corticosteroids: Anti-inflammatory medications used to reduce itching and inflammation.
- Topical calcineurin inhibitors: Anti-inflammatory medications used to treat moderate-to-severe eczema.
- Systemic immunosuppressants: Suppress the immune system and can be used to treat severe cases of eczema.
- Light therapy: It involves exposing the skin to specific wavelengths of light to reduce inflammation and itching.
- Wet wraps: This involves wrapping the affected area in a damp layer of fabric to help hydrate the skin and reduce inflammation.
- Behavioral interventions: This includes stress management techniques, such as relaxation exercises or cognitive-behavioral therapy, which can help reduce stress and improve symptoms.
Outlook:
It is important to note that while no cure exists for atopic dermatitis (AD), suitable treatment options are available to manage flares, subside symptoms and improve quality of life. The outlook of symptoms expected to arise varies in severity and duration depending on exposure to risks. Keeping track of what accentuates the condition can help you figure out the potential risks associated with the flare-up. With the right treatment and wholesome care, most people with atopic dermatitis (AD) can lead a full and active life.
Additionally, volunteering in clinical trials in Michigan enables your access to novel treatment options to better manage your condition.